|
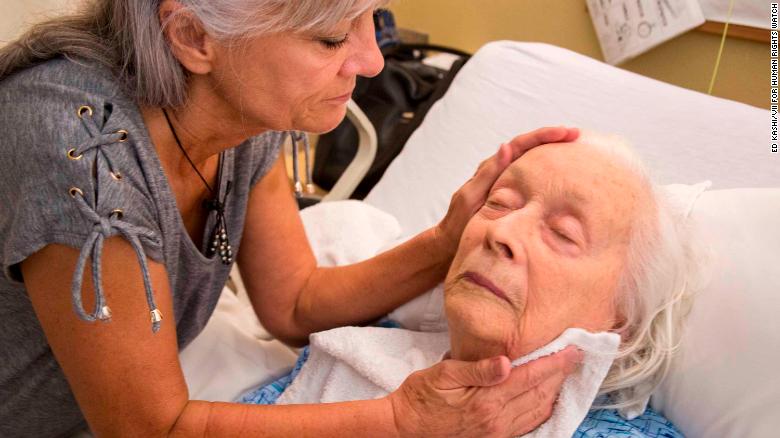
Lenora Cline, 88, has lived in a nursing home for years. She has
Alzheimer’s disease. Laurel Cline, her daughter, visits her twice a day
and assists staff with the care-taking, fearing that otherwise, with the
shortage of staff, her mother will not be turned, fed, or changed. She
had to persuade the facility to discontinue antipsychotic medications.
Before successfully objecting to their use, Ms. Cline said, “Every
little thing, they want to put you on psych meds.” Los Angeles,
California, August 2017.
© 2017 Ed Kashi for Human Rights Watch |
In an average week, nursing facilities in the United States
administer antipsychotic drugs to over 179,000 people who do not have
diagnoses for which the drugs are approved. The drugs are often given
without free and informed consent, which requires a decision based on a
discussion of the purpose, risks, benefits, and alternatives to the
medical intervention as well as the absence of pressure or coercion in
making the decision. Most of these individuals—like most people in
nursing homes—have Alzheimer’s disease or another form of dementia.
According to US Government Accountability Office (GAO) analysis,
facilities often use the drugs to control common symptoms of the
disease.
While these symptoms can be distressing for the people who experience
them, their families, and nursing facility staff, evidence from
clinical trials of the benefits of treating these symptoms with
antipsychotic drugs is weak. The US Food and Drug Administration (FDA)
never approved them for this use and has warned against its use for
these symptoms. Studies find that on average, antipsychotic drugs almost
double the risk of death in older people with dementia. When the drugs
are administered without informed consent, people are not making the
choice to take such a risk.
The drugs’ sedative effect, rather than any anticipated medical
benefit, too often drives the high prevalence of use in people with
dementia. Antipsychotic drugs alter consciousness and can adversely
affect an individual’s ability to interact with others. They can also
make it easier for understaffed facilities, with direct care workers
inadequately trained in dementia care, to manage the people who live
there. In many facilities, inadequate staff numbers and training make it
nearly impossible to take an individualized, comprehensive approach to
care. Many nursing facilities have staffing levels well below what
experts consider the minimum needed to provide appropriate care.
Federal regulations require individuals to be fully informed about
their treatment and provide the right to refuse treatment. Some state
laws require informed consent prior to the administration of
antipsychotic drugs to nursing home residents. Yet nursing facilities
often fail to obtain consent or even to make any effort to do so. While
all medical interventions should follow from informed consent, it is
particularly egregious to administer a drug posing such severe risks and
little chance of benefit without it.
Such nonconsensual use and use without an appropriate medical
indication are inconsistent with human rights norms. The drugs’ use as a
chemical restraint—for staff convenience or to discipline or punish a
resident—could constitute abuse under domestic law and cruel, inhuman,
and degrading treatment under international law.
The US has domestic and international legal obligations to protect
people who live in nursing facilities from the inappropriate use of
antipsychotic drugs, among other violations of their rights. These
obligations are particularly important as people in nursing facilities
are often at heightened risk of neglect and abuse. Many individuals in
nursing facilities are physically frail, have cognitive disabilities,
and are isolated from their communities. Often, they are unable or not
permitted to leave the facility alone. Many depend entirely on the
institution’s good faith and have no realistic avenues to help or safety
when that good faith is violated.
US authorities, in particular the Centers for Medicare & Medicaid
Services (CMS) within the US Department of Health and Human Services,
are failing in their duty to protect some of the nation’s most at-risk
older people. On paper, nursing home residents have strong legal
protections of their rights, but in practice, enforcement is often
lacking. Although the federal government has initiated programs to
reduce nursing homes’ use of antipsychotic medications and the
prevalence of antipsychotic drug use has decreased in recent years, the
ongoing forced and medically inappropriate use of antipsychotic drugs
continues to violate the rights of vast numbers of residents of nursing
facilities. The US government should use its full authority to enforce
longstanding laws, including by penalizing noncompliance to a degree
sufficient to act as an effective deterrent, to end this practice.
This report documents nursing facilities’ inappropriate use of
antipsychotic drugs in older people as well as the administration of the
drugs without informed consent, both of which arise primarily from
inadequate enforcement of existing laws and regulations. The report is
based on visits by Human Rights Watch researchers to 109 nursing
facilities, mostly with above-average rates of antipsychotic medication
use, between October 2016 and March 2017 in California, Florida,
Illinois, Kansas, New York, and Texas; 323 interviews with people living
in nursing facilities, their families, nursing facility staff,
long-term care and disability experts, officials, advocacy
organizations, long-term care ombudsmen, and others; analysis of
publicly available data; and a review of regulatory standards,
government reports, and academic studies.
This report is especially relevant at this time because the US is
aging rapidly. Most of the people in the nursing facilities Human Rights
Watch visited are over the age of 65. Older people now account for one
in seven Americans, almost 50 million people. The number of older
Americans is expected to double by 2060. The number of Americans with
Alzheimer’s disease, the most common form of dementia, is expected to
increase from 5 million today to 15 million in 2050. The system of
long-term care services and supports will have to meet the needs—and
respect the rights—of this growing population in coming years.
Social Harm and Health Risks Caused by Antipsychotic Drugs Used Unnecessarily or as Chemical Restraints
The American Psychiatric Association (APA) Practice Guideline on the
Use of Antipsychotics to Treat Agitation or Psychosis in Patients with
Dementia states that, after eliminating or addressing underlying
medical, physical, social, or environmental factors giving rise to
manifestations of distress associated with dementia, antipsychotic drugs
“can be appropriate” as a means to “minimize the risk of violence,
reduce patient distress, improve the patient’s quality of life, and
reduce caregiver burden.” However, given the “at best small” potential
benefits and the “consistent evidence that antipsychotics are associated
with clinically significant adverse effects, including mortality,” it
is essential that the drug treatment is only attempted when appropriate.
Nursing facility staff, individuals living in facilities, their
families, long-term care advocates, and others told Human Rights Watch
that the drugs are not used only as a last resort, after all factors
potentially giving rise to a person’s distress have been ruled out, and
after nonpharmacologic interventions have been attempted unsuccessfully.
Instead, antipsychotic drugs are used sometimes almost by default for
the convenience of the facility, including to control people who are
difficult to manage.
One facility social worker said that one of the most common
“behaviors” leading to antipsychotic drug prescriptions was someone
constantly crying out, “help me, help me, help me.” An 87-year-old woman
reflected that at her prior facility, which gave her antipsychotic
drugs against her will, “they just wanted you to do things just the way
they wanted.” A social worker who used to work in a nursing facility
said the underlying issue is that “the nursing homes don’t want
behaviors. They want docile.” A state surveyor said: “I see way too many
people overmedicated.... [Facilities] see it as a cost-effective way to
control behaviors.”
Human Rights Watch interviewed people who live in nursing homes and
their family members who described the harmful cognitive, social, and
emotional consequences of the medications that all too often should
never have been administered in the first place: sedation, cognitive
decline, fear, and frustration at not being able to communicate. Most or
all antipsychotic drugs are associated with sedation and fatigue in
people with dementia.
A 62-year-old woman in a nursing facility in Texas who said she was
given Seroquel, a common antipsychotic drug, without her knowledge or
consent said: “[It] knocks you out. It’s a powerful, powerful drug. I
sleep all the time. I have to ask people what the day is.” The daughter
of a 75-year-old woman in Kansas said that when the nursing facility
began giving her mother an antipsychotic drug, her mother “would just
sit there like this. No personality. Just a zombie.... The fight is
gone.”
Nursing staff, social workers, long-term care ombudsmen, and state
surveyors echoed this perception. One director of nursing said: “You
actually see them decline when they’re on an antipsychotic. I think it’s
sadder than watching someone with dementia decline.”
Lack of Informed Consent Prior to Antipsychotic Medication Administration
The use of antipsychotic drugs to control people without their
knowledge or against their will in nonemergency situations violates
international human rights. The practicalities of obtaining consent from
an older person with dementia can be fraught. However, in many of the
cases Human Rights Watch documented, nursing facilities made no effort
to obtain meaningful, informed consent from the individual or a health
proxy before administering the medications in cases where it clearly
would have been possible to do so.
Our research suggests that in many other cases, facilities that
purport to seek consent fail to provide sufficient information for
consent to be informed; pressure individuals to give consent; or fail to
have a free and informed consent procedure and documentation system in
place. Under international human rights law, in the absence of free and
informed consent, a nonemergency medical intervention that is not
necessary to address a life-threatening condition is forced treatment.
One former nursing facility administrator explained:
The facility usually gets informed consent like this: they
call you up. They say, “X, Y, and Z is happening with your mom. This is
going to help her.” Black box warning (the government’s strongest
warning to draw attention to serious or life-threatening risks of a
prescription drug)? “It’s best just not to read that.” The risks? They
gloss over them. They say, “That only happens once in a while, and we’ll
look for problems.” We sell it. And, by the way, we already started
them on it.
A current director of nursing admitted, “We are supposed to be doing
informed consent. It’s on the agenda. But really antipsychotics are a
go-to thing. ‘Give ‘em some Risperdal and Seroquel.’ We tell the family
as we’re processing the order. The family is notified.” The daughter of a
woman in a nursing facility described having consented to antipsychotic
drugs for her mother without understanding the risks: “I had no idea,
not at all, that the drugs were dangerous. I had
no idea.... I’m guessing most people have no idea.”
A detailed examination of the question of legal capacity—the right to
exercise one’s own rights and to make decisions on one's own behalf—is
outside the scope of this report. Because many people living in nursing
facilities have dementia and other progressive conditions that affect
their cognitive ability, it is a highly complex question how medical and
other decisions concerning their care should be made in a
rights-respecting manner. In US nursing facilities, substituted
decision-making—where a family member or other third party, whether
voluntarily designated in advance or not, makes decisions on an
individual’s behalf—is common.
Government Obligations
In 2012, CMS created the National Partnership to Improve Dementia
Care in Nursing Homes, in recognition of the unacceptably high
prevalence of antipsychotic drug use. While the initiative—which set
targets for the industry to reduce antipsychotic drug rates—may have
contributed to the reduction of the use of antipsychotic medications
over the last six years, it cannot substitute for the effective
regulation of nursing homes, including by ensuring that facilities face
meaningful sanctions for noncompliance with mandatory standards. Our
research found that CMS is not using its full authority to address this
issue. Recently, CMS is in fact moving in the opposite direction,
limiting the severity of financial penalties and the regulatory
standards with which facilities must comply.
CMS and the state agencies with which it contracts to enforce federal
regulations are not meeting their obligation to protect people from the
nonconsensual, inappropriate use of antipsychotic drugs. Human Rights
Watch identified several key areas of concern:
- Failure to adequately enforce the
right to be fully informed and to refuse treatment or to require free
and informed consent requirement. The Nursing Home Reform Act of 1987
grants residents the right “to be fully informed in advance about care
and treatment,” to participate in care planning, and to refuse treatment
without penalty. If it were enforced fully, these protections would not
differ substantially from the right to free and informed consent.
However, without adequate enforcement, current practice falls far short
of this protection.
- Lack of minimum staffing
regulations. Adequate numbers of sufficiently competent staff are at the
crux of nursing facility care. Yet government regulations do not set a
minimum staffing requirement for nursing facilities, instead requiring
that facilities determine for themselves what amounts to “sufficient”
and “competent” staff for their residents. While experts put minimum
adequate nursing staffing time at 4.1 to 4.8 hours per resident per day,
most facilities self-reported to the government providing less than
that; almost one thousand facilities self-reported providing less than
three hours of staff time per day.
- Weak enforcement of federal
regulations specifically banning chemical restraints and unnecessary
drugs. Federal regulations prohibit chemical restraints—drugs used for
the convenience of staff or to discipline residents without a medical
purpose—and unnecessary drugs: a technical term meaning drugs used
without adequate clinical indication, monitoring, or tapering. The
regulations also provide for the right to refuse treatment. However,
federal and state enforcement of these regulations is so weak that the
drugs are routinely misused without significant penalty. Almost all
antipsychotic drug-related deficiency citations in recent years have
been determined to be at the level of causing “no actual harm,”
curtailing the applicability and severity of financial sanctions.
With such vast numbers of nursing facility residents still getting
antipsychotic drugs that many do not need, do not want, and that put
their lives and quality of life at risk, federal and state governments
need to do more to ensure that the rights of residents are adequately
protected. An industry entrusted to provide care—and paid billions of
public and private dollars to do so—cannot justify compounding the
vulnerabilities, challenges, and loss that people often experience with
dementia and institutionalization.
Full Article & Source:
How Nursing Homes in the United States Overmedicate People with Dementia