BISHOP,
Calif. — When Jamie Moore arrived home on a Thursday evening in March,
she was surprised to find her mother-in-law in her living room. Glenda
Moore, 67, had been sitting in her wheelchair for hours. Without anyone
to help her to the bathroom, she’d had an accident. She was also having
trouble breathing. “It was awful,” Jamie Moore recalled.
Glenda
Moore told Jamie that she had been discharged from the Bishop Care
Center nursing home, in Bishop, California. She had been living at the
nursing home — a sprawling brick building on the side of a state highway
— for several weeks, recovering from a back surgery that unexpectedly
left her unable to walk much or take care of herself.
Several
days earlier, nursing home administrators had shown Glenda Moore a
letter from Medicare, explaining that her rehabilitation coverage was
ending. She was unable to pay the nursing home’s more-than-$7,000
monthly fee, so, thinking she had no other options, she left. (A
relative dropped her off at Jamie’s home, where Glenda Moore had lived
previously, without telling Jamie.)
“They
pushed her out and she was not ready,” Jamie Moore, who has worked as a
nursing assistant, said. “She was not ready at all.”
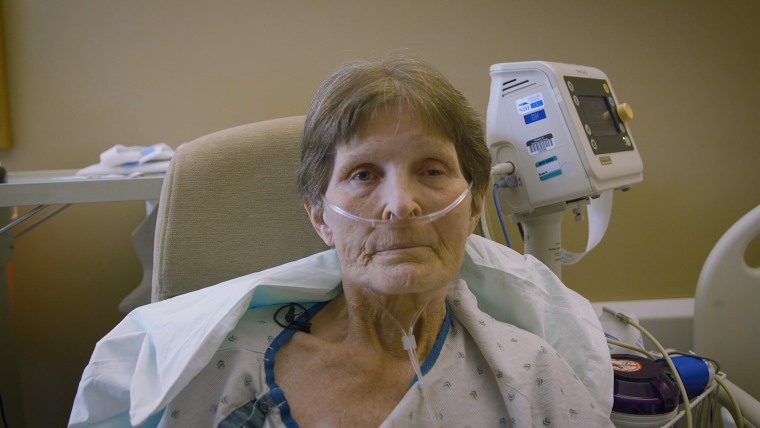
As
the family later learned, Glenda Moore had the right to appeal the
Medicare decision, or to apply for Medicaid — and, if she qualified
(which she later did), to stay in the nursing home on Medicaid for as
long as she needed nursing care. Instead, Moore’s family said, Moore
became one of thousands of Americans discharged against their wishes or
evicted from nursing homes each year. (The Bishop Care Center maintains
that Moore's health had improved and that she voluntarily left the
facility, and points out that they gave her a document noting her right
to appeal the Medicare decision.)
Nationally,
long-term care ombudsmen, who advocate for elderly and disabled
residents of nursing homes and assisted living facilities, received
10,610 complaints about discharges and transfers in 2017, up from 9,192
in 2015. The ombudsmen, whose work is federally mandated and
state-funded, receive more complaints about discharges and transfers than any other grievance.
The
complaints likely expose just a small fraction of the problem, said
Kelly Bagby, vice president at the AARP Foundation, a nonprofit that
serves vulnerable people over 50.
“Most people don’t even know they have rights,” she said. And many complaints never result in a formal state investigation.
Advocates, experts and the federal government
say that nursing homes tend to evict low-income, longer-term residents
who receive Medicaid, to make room for shorter-term rehabilitation
patients who are covered by Medicare. Medicare reimburses nursing homes
at a higher rate than Medicaid, so it’s more lucrative for facilities to
house Medicare patients who stay for short stints before recovering and
moving elsewhere.
In California, for example, the average state
Medicaid reimbursement for a nursing home is $219 per day, according to
the California Association of Health Facilities, while Medicare may
reimburse more than $1,000 per day, but only for up to 20 days, when
patients must begin paying part of the fees. (Medicare coverage ends
completely after 100 days.) Advocates say that eviction notices are
often handed out around the 20-day mark.
“It
is illegal to discriminate against residents based on payment source,
but it happens all the time,” said Tony Chicotel, attorney at the
California Advocates for Nursing Home Reform, a nonprofit that supports
long-term care residents in the state. “It feels like there’s just a
tidal wave of cases.”
Chicotel said he
receives calls every day from panicked residents or family members being
threatened with discharge from a long-term care facility.
Deborah
Pacyna, director of public affairs at the California Association of
Health Facilities, a trade association representing nursing homes, told
NBC News that improper and illegal discharges are “a really rare thing,”
and that the issue is exaggerated by media attention.
She
added that California’s Medicaid program, Medical, does not provide
“adequate funding” to care for many patients with complicated health
issues and behavioral disorders. “Medicare pays more. Those people are
rehab patients; they’re in and out,” she said. “That is how they break
even,” she added of nursing homes. “Society’s problems are manifesting
themselves on the doorsteps of nursing homes.”
‘You’re just a piece of garbage’
Nursing homes are legally permitted to evict residents under several conditions:
if a resident’s health improves sufficiently; if his presence in a
facility puts others in danger; if the resident’s needs cannot be met by
the facility; if he stops paying and has not applied for Medicare or
Medicaid; or if the facility closes. Facilities are obligated under
federal law to give 30 days’ notice, in writing, and also to work with
the resident on a transition plan.
Bagby,
of the AARP, said that while some residents are issued formal discharge
letters with advance notice, others are asked or pressured to leave with
“no due process rights, no notice.”
In one
case in Los Angeles, in April 2018, Ronald Anderson said he was woken
at night by the nursing home staff at the Avalon Villa Care Center and
told he was being evicted. Anderson, 51 at the time, had moved into the
facility over a year earlier to recover from a partial foot amputation.
He said he was loaded into a van and dropped off on a sidewalk in
downtown Los Angeles, which has one of the largest homeless populations
in the country, according to a report from the California Department of Public Health.
Anderson,
who is diabetic, was left in a wheelchair without his insulin or
testing supplies — on a street cluttered with tent encampments and
broken glass. The Department of Public Health report noted that he could
have slipped into a coma or died.
“You’re
just a piece of garbage,” Anderson said, from the Union Rescue Mission
homeless shelter in Los Angeles where he now lives. “They’ll kick you
right out on the curb.”

Avalon Villa Health Care, which runs the nursing home, later paid $450,000 to settle a civil complaint
filed by the Los Angeles city attorney in response to Anderson’s case
and other evictions of homeless residents, with the money going toward
civil penalties, hiring and training Avalon Villa staff and finding
temporary housing for the facility’s homeless residents. The city
attorney set up an emergency hotline and invited members of the public
to report cases of resident abandonment.
A
lawyer for the Avalon Villa Care Center told NBC News that the facility
“strongly disputes that it has inappropriately discharged any patients”
and “rejects the allegations of the city attorney.”
The
Rev. Andy Bales, director of the Union Rescue Mission, said “resident
dumping” from nursing homes and hospitals is so common that the shelter
set up a security camera outside — which Bales calls “the dump cam” — to
capture evidence of it. He said he is aware of at least four instances
from the last year in which people have been dropped off on nearby
streets by hospitals or nursing homes — though he believes the number is
higher. As a result of the security camera, he said, “They won’t dump
them off in front of us anymore.”
California’s long-term care ombudsmen received 1,404 complaints about nursing home evictions in 2018, up from 1,022 in 2014. Several lawsuits concerning nursing home discharges have recently been filed in the state.
Molly
Davies, a California long-term care ombudsman, said that in addition to
receiving more complaints about evictions, “there has also been an
uptick in the egregiousness of some of these cases.”
In some
instances, she and other experts said, nursing homes drop residents off
at a low-cost motel and pay for a night or two. “We’ve seen cases with
residents who have dementia put into a van and dropped downtown onto the
streets, without the ability to care for themselves,” she said.
The California Department of Public Health
does not track where nursing homes discharge patients, according to a
department spokesman, nor does the California long-term care ombudsman
program. In some instances, however, routine state inspections and
inspections following complaints uncover problems.
In
a 2018 incident, described in a California Department of Health and
Human Services report, a Rosemead nursing home discharged a resident to a
hotel without any medical equipment and without ensuring that the hotel
was “a safe environment.” The female resident still required assistance
with activities such as using the toilet and bathing, and was found to
lack “the capacity to make her needs known.” The nursing home received a
federal “deficiency” citation.
In another case that resulted in a deficiency citation,
a nursing home resident who “needed extensive assistance” to move
between locations in his bedroom was discharged to a motel — and, a few
days later, ended up in a hospital for emergency care.
These
practices are not unique to California. In Maryland, one nursing home
resident was dropped off in Baltimore, a city she had never been to,
according to the state attorney general’s office. In another instance, a
Washington County Sheriff’s deputy accused a nursing home of discharging a resident to a storage unit on a hot summer day.
Even
when residents appeal eviction decisions through a state process and
win the right to return to a nursing home, that nursing home sometimes
refuses to readmit them, a group of plaintiffs told the Ninth Circuit
Court of Appeals found in July. The case is still pending, but the
appeals court agreed with the plaintiffs that federal law does not allow
“meaningless show trials that allow nursing homes to persist in
improper transfers and discharges.”
The
California Department of Health Care Services, the California Department
of Public Health and the federal Centers for Medicare & Medicaid
Services all declined to comment, citing department policy not to
comment on pending litigation.
A push for enforcement
In 2016, the Centers for Medicare & Medicaid Services strengthened regulatory requirements around nursing home discharges and transfers, specifying
that residents cannot be evicted for nonpayment while they are in the
process of applying for Medicaid or appealing a Medicaid denial. A year
later, the agency announced an initiative
to prevent illegal nursing home discharges, acknowledging that “some
discharges are driven by payment concerns, such as when Medicare or
private pay residents shift to Medicaid as the payment source.”
So
far, the agency has approved $784,630 for a program in California that
focuses on training nursing home staff on discharge regulations, a
spokeswoman said in an email. The agency also provided $84,00 for a
smaller project in Montana. Beyond that, the agency is not acting
directly to address illegal evictions but is instead encouraging states
“to propose projects that seek to address facility-initiated discharges
that violate federal regulations,” the spokeswoman said by email.
Advocates
for nursing home patients said more is needed. They want both federal
and state agencies to do more to enforce existing rules on evictions.
“We
haven’t seen any change in practice,” said Davies, the California
long-term care ombudsman. “We haven’t seen a reduction in inappropriate
transfers and discharges. There are certain enforcement tools that they
have that they aren’t using consistently.” These tools, she said,
include substantial fines.
But the federal government has made changes that reduced
fines against nursing homes that harm or endanger residents. Nursing
homes used to receive fines for each day a violation was observed, but
after a change the Trump administration implemented in July 2017,
nursing homes are now usually fined just once per retroactive violation.
Robyn
Grant, director of public policy and advocacy at the National Consumer
Voice for Quality Long-Term Care, an advocacy group, says this change
can affect the way illegal evictions are punished. For instance, a
nursing home that evicts a patient and refuses to readmit the person may
be fined one time, instead of every day that the resident is denied
access to a bed.
In the first 18 months
following the change in guidelines, nursing homes across the country
paid about $47 million less in fines for all violations compared to the
previous 18-month period, said Dr. David Gifford, senior vice president
of quality and regulatory affairs at the American Health Care
Association, the nursing home industry’s main lobbying group.
Gifford
told NBC News that the change was not about saving the industry money,
but was meant to ensure consistent standards. He said the new fine
structure incentivizes nursing homes to report violations and improve
resident care.
‘I thought I was completely covered’
After
she left the Bishop Care Center nursing home in March, Glenda Moore
grew sicker. Over the following weeks, she cycled among her son and
daughter-in-law’s home, several emergency rooms and another nursing home
an hour away. According to her son and daughter-in-law, she was
diagnosed with a bladder infection and pneumonia.
“I
don’t want to be a burden on the kids,” Glenda Moore told NBC News in
an interview in April. “I had retirement insurance, I had Medicare, I
thought I was completely covered. That doesn’t count for anything … I
had no idea.”
In May, her family appealed
her discharge from the center. At a hearing conducted by the California
Department of Health Care Services, the nursing home’s administrator
said Glenda Moore had left willingly, according to the state’s summary
report.
The state’s hearing officer
ultimately found that the facility “failed to meet all of the
regulatory-mandated discharge planning requirements.” However, the
hearing officer ruled in favor of the nursing home, noting that Glenda
Moore agreed to leave and was given paperwork notifying her of her right
to appeal Medicare’s noncoverage decision.
By
late July, her weight had dropped to about 80 pounds. She was
hospitalized, and on Aug. 2 she died from acute renal failure and
cardiopulmonary arrest.

Her
family believes she wouldn’t have become so sick if she had been able
to stay in the Bishop Care Center for a few weeks longer, until she was
more stable.
Jamie Moore said her mother-in-law’s experience has changed the way she thinks about her own retirement.
Full Article & Source:
Some nursing homes are illegally evicting elderly and disabled residents who can't afford to pay

No comments:
Post a Comment