For older people, loneliness and the stress of weighing risk of ordinary activities have taken an additional toll
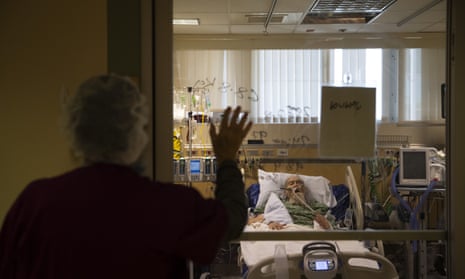
It was Mother’s Day in May 2020, and an elderly woman lay dying in a Rhode Island nursing home. Her children couldn’t visit because of Covid, and as much as Adelina Ramos, her certified nursing assistant, longed to provide comfort from her bedside, she had to leave, even though she could see the woman was slipping away.
She had 25 other patients to care for that day.
It “really broke my heart,” Ramos said. “Families trust us to care for their loved ones. I can’t describe how painful it feels when we are forced to make those kinds of choices.”
She recounted the devastation wrought by the pandemic in a hearing on Wednesday before the House subcommittee on the coronavirus crisis.
Although Covid causes less panic now, particularly given the protection offered by updated vaccines and treatments, older Americans are still seeing their lives upended – and, tragically, ended entirely – by new outbreaks.
As the rest of the country seeks a new normal, millions of vulnerable Americans still remain at risk and in limbo. They’re now navigating a world ruptured by continued virus surges, shortages in the staff who care for them, and grief over more than a million people lost in two years.
Even so, the US Centers for Disease Control and Prevention (CDC) on Friday dropped its mask recommendations for hospitals and nursing homes, except during times of high transmission or while providers are caring for moderately and severely immune-compromised patients.
The move could make it even more difficult for those at risk, especially elderly people, to navigate health care settings and long-term care facilities safely.
Prioritizing older Americans during this time is “paramount”, said David Grabowski, a professor of health care policy at Harvard Medical School. “It’s the group overall during the pandemic that’s been hit the hardest, and yet in many ways … they’ve been an afterthought.”
People over the age of 50 account for more than 93% of Covid deaths in the US.
“We still are seeing hundreds of deaths a day, and they’re occurring disproportionately among older Americans,” said Theresa Andrasfay, a postdoctoral scholar of gerontology at the University of Southern California.
Life expectancy has dropped for all Americans, but changes are greater among communities of color, Andrasfay said. “The Native American population had by far the largest decline in life expectancy, followed by the Latino population and then the Black population.”
In February 2021, older Americans who caught Covid were 1,000 times more likely to die than teenagers, according to a McKinsey report that predicted the “arrival of safe, effective vaccines makes the pain of that isolation a time-bound problem”.
Yet for many, isolation and stress from the pandemic persist, especially as the protection offered by vaccines wanes without boosters and as new variants emerge.
Relatively high rates of vaccinations among older people helped mortality rates drop slightly in this age group from 2020 to 2021. But the Omicron variant, which is more transmissible and better at evading immunity, brought near-record surges in elderly mortality.
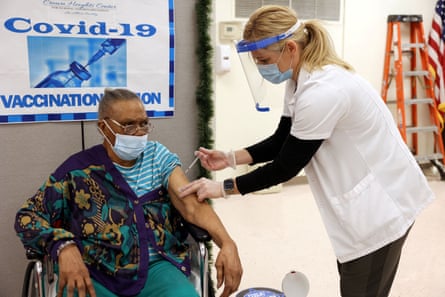
A total of 95% of Americans above the age of 65 have gotten at least one Covid shot. But from there, the coverage begins to drop precipitously. Among those who were fully vaccinated in this age group, 70.8% got their first boosters. But only 40% of that group went on to get second boosters.
That means a total of 14.9 million older Americans are up-to-date on vaccinations, compared with the 57.5 million who were willing to get the first shot. Booster rates are even lower among Americans aged 50 to 64.
This could have dire implications for their safety moving forward, even as remaining precautions disappear across the country.
In nursing homes, only 57% of residents and 43% of staff are up to date on their vaccines. Rates are lowest in Arizona, Florida, Nevada and Texas.
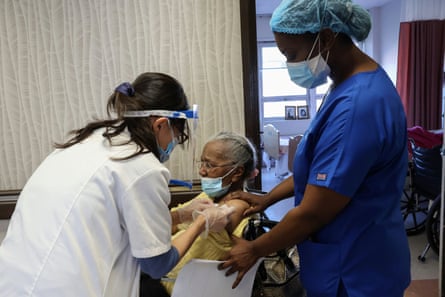
Fewer than 1% of Americans live in long-term care facilities, yet about one-fifth of all deaths from Covid-19 are related to nursing homes, with more than 200,000 residents and workers dying from the coronavirus since the start of the pandemic.
“Residents, their families and their caregivers have long known that US nursing home care is broken, yet this issue has gone largely unnoticed in the broader population. Covid changed this,” Grabowski testified at the hearing.
The House coronavirus subcommittee outlined the “dire” conditions of for-profit nursing homes during the early months of the pandemic, revealing widespread neglect that led to health deterioration and death.
Nurses and nursing aides cared for as many as 38 patients during their shifts. In April 2020, when only one nurse was covering two entire floors at a facility in Nevada, one resident waited four hours for a sip of water and another resident who vomited on herself was not cleaned for at least two days, according to the House report.
Yet at least 32 states have passed legislation making it harder for residents or their families to sue long-term care facilities for such treatment.
Some of the worker shortages were because of Covid cases among staff, which could have been prevented in part with better precautions. But one nursing home worker alleged that the corporations wanted to save money by not hiring additional workers despite the need for them.
Long-term care facilities were plagued with staffing shortages and low morale before the pandemic started, and Covid sharply amplified the cracks in how America cares for its senior population.
“Nursing homes are already understaffed, under-resourced. So when you’re putting a profit motive on nursing homes to squeeze out a couple extra dollars from these communities, it’s going to compromise care,” said Ashwin Kotwal, assistant professor of geriatrics at the University of California, San Francisco, School of Medicine.
But it’s not only nursing home residents who have been affected by Covid – and damage from the pandemic wasn’t limited to the virus itself.
The pandemic also caused stress and loneliness, which affects both mental and physical health. In 2019, about 1.6 million adults above the age of 70 were homebound, but that number more than doubled to 4.2 million in 2020. Being homebound increases the risks of sickness and death.
Age was the greatest risk factor for severe outcomes from Covid, but loneliness compounded poor health, according to a Commonwealth Fund survey conducted between March and June 2021. Pandemic disruptions limited and delayed health care, and it amplified “considerable” social and economic challenges.

“Compared to their counterparts in the other survey countries, older adults in the US have suffered the most economically from the Covid-19 pandemic, with more losing a job or using up all or most of their savings,” the report said. Economic hardships for older Americans were four to six times greater than in other countries surveyed, and they were more likely among Latino and Black adults than among white adults in the US.
Disruption and isolation are likely to continue for those who need to continue taking Covid precautions.
“What’s concerning going forward, as there’s more focus on individual responsibility, is that it makes it more difficult for people who are vulnerable, either because of underlying conditions or because of their age, to feel safe taking part in necessary activities,” Andrasfay said.
Those activities can include taking public transportation, medical visits, returning to work or seeing family and friends.
Weighing these risks is a fraught and exhausting process, Kotwal said.
“It can make even the most simple of social activities something that people really stress over and think about a lot. I’ve seen a lot of anxiety around how people make these decisions to do what are really normal activities, like going to grab coffee with their child or hanging out with their grandchildren.”
Keeping up-to-date on vaccines is an important part of protecting those most at risk, he said. “We can bring this into a place of community – being responsible, trying to protect others – rather than only looking at this from the individual safety lens.”
Vaccination clinics and vaccine mandates in health systems and long-term care facilities were “really effective,” Grabowski said. About 87% of residents and staff in nursing homes were vaccinated because of the clinics and mandates – but those requirements have not been updated to include boosters.
An expanded federal mandate for staff to receive booster doses would help, he said. And more vaccine clinics for facilities, as well as campaigns to reach homebound adults and others facing access problems, could also increase booster rates and protect older adults this winter.
“This is too important,” Grabowski said. “By all means, let’s make this as easy as possible.”
Full Article & Source:
‘They’ve been an afterthought’: millions of elderly Americans still vulnerable as pandemic caution wanes






















